Campaign to Reduce Opioid Prescribing (CROP)
CROP was designed to assist general practices across West Yorkshire with opioid deprescribing in an effort to improve patient care and safety across the region.
Study team:
-
Dr Sarah Alderson, Clinical Lecturer in Primary Care & NIHR Clinical Trials Fellow, University of Leeds
-
Professor Robbie Foy, Clinical Professor of Primary Care, University of Leeds
-
Dr Thomas Willis, Senior Research Fellow, University of Leeds
-
Dr Su Wood, Research Fellow, University of Leeds
-
Dr Tracey Farragher, Lecturer in Healthcare Sciences, University of Manchester
CROP was the first in a series of audit and feedback projects that focused on deprescribing across the region. You can read about the other projects below:
-
CROP - The Campaign to Reduce Opioid Prescribing
-
RETHINK - A project aiming to reduce prescribing for neuropathic pain through audit and feedback
-
LAMP - A project focusing on lowering antimicrobial prescribing
Summary:
Opioid medicines, such as codeine or morphine, work well for short-lived pain (e.g. following injury) and cancer pain. They may not work and can be harmful in chronic pain. There is concern that patients with chronic pain are being given more and stronger opioids without trying other, less harmful options.
A local study1 funded by the National Institute for Health Research (NIHR) under its Research for Patient Benefit Programme (RfPB) found that opioid prescribing for chronic non-cancer pain by General Practitioners (GPs) in Leeds and Bradford doubled over 2005-12 and strong opioids increased six-fold. There were large differences in prescribing between practices, suggesting that opioid prescribing is driven by GP habits rather than patient need.
The aim of this transformational project was not to try to reduce opioid prescribing but to try not to increase the current rate any further, i.e. to create a plateau in opioid prescribing which would represent an efficiency gain of approximately £500k. However the results achieved indicated that in fact prescribing did not just plateau, it actually went down. Over the 12 month project period total prescribing of opioids for non-cancer pain fell by 5.14% across the West Yorkshire region, with a decrease in opioid prescribing in every area.
Figure 1. % Change in opioids items per 1000 patients during CROP
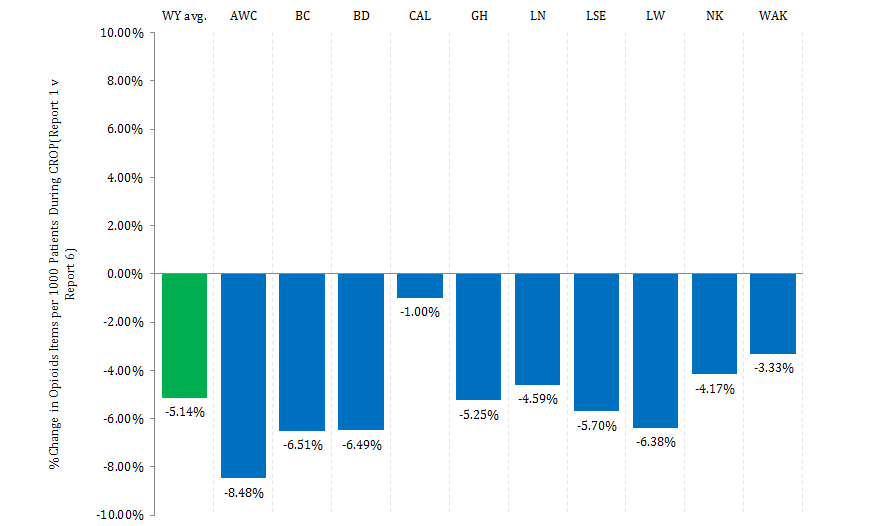
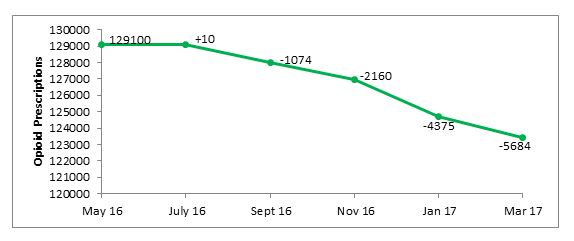
Figure 2. Opioids prescriptions dispensed in West Yorkshire during the CROP period
You can view a presentation about CROP online, recorded in December 2021: De/Implement: Experiences from the UK of Avoiding Unnecessary Opioid Prescribing in Primary Care Using Enhanced Feedback
Please contact us if you have any questions: research@bradford.nhs.uk
Further reading
-
The effects of an evidence- and theory-informed feedback intervention on opioid prescribing for non-cancer pain in primary care: a controlled interrupted time series analysis - Sarah L. Alderson, Tracey M. Farragher, Thomas A. Willis, Paul Carder, Stella Johnson, Robbie Foy
-
General practice responses to opioid prescribing feedback: a qualitative process evaluation - Su Wood, Robbie Foy, Thomas A Willis, Paul Carder, Stella Johnson, Sarah Alderson
-
Embedded trials within national clinical audit programmes: a qualitative interview study of enablers and barriers - Sarah Alderson, Thomas A. Willis, Su Wood, Fabiana Lorencatto, Jill Francis, Noah Ivers, Jeremy Grimshaw, Robbie Foy